Glaucoma specialist Melbourne
Everything you need to know about glaucoma and glaucoma treatment
Glaucoma occurs when high eye pressure causes progressive damage to your optic nerve, resulting in irreversible vision loss. The key is to detect glaucoma early and start treatment before any significant sight loss has occurred. Most patients with glaucoma are treated with eye drops or laser, or a combination of both. In some cases, however, glaucoma surgery may be recommended.
Eye surgeon Melbourne
Dr Brian Ang in a nutshell
In United Kingdom, Switzerland, New Zealand and India
Glaucoma symptoms
What is glaucoma?
Before we answer that question, let’s use the analogy of
- the eyeball being a camera,
- the brain being a computer,
- and the optic nerve being the cable that connects the eyeball (camera) to the brain (computer).
To be able to see, all 3 components need to function well.
Glaucoma is a disease whereby pressure within the eyeball (camera) causes progressive and irreversible damage to the optic nerve (the connecting cable). This optic nerve damage will cause you to gradually lose your peripheral vision, giving you a progressively worsening tunnel vision effect.
Glaucoma specialist Melbourne
"The reason there is pressure in the eye is because of a fluid called aqueous. Aqueous is constantly produced to provide nutrients to the cells of the eye, and also constantly drained to take away waste material from the same cells. Eye pressure is increased when there is build up of aqueous in the eye due to inadequate drainage."
Once glaucoma has already damaged your vision, there is no treatment that will be able to restore the damage or recover your vision fully. It is therefore crucial to detect glaucoma early and to start treatment before any significant vision loss has already occurred. Most people with glaucoma, when detected early and managed appropriately, retain useful vision for the rest of their lives.
"My job as a glaucoma specialist is to work with you to minimise vision loss from glaucoma so that you can maintain your best possible vision for the rest of your life."
Dr Brian Ang Glaucoma specialist Melbourne
Glaucoma is fairly common, affecting up to 2% of the population. In Australia, it is estimated that over 300,000 people suffer from glaucoma. Glaucoma is the leading cause of irreversible blindness in Australia and worldwide.
Can I prevent glaucoma?
Unfortunately, there is no guaranteed way to prevent glaucoma. The most important thing is to be aware of your risk of glaucoma and to be monitored regularly by an eye care professional (optometrist or ophthalmologist).
Risk factors include:
- A family history of glaucoma
- Previous ocular trauma
- Prolonged use of steroid medication
- Known high eye pressure
It is a good idea to have your eyes checked at least once a year once you hit the age of 50, or earlier if you have risk factors.
If you are a glaucoma suspect, it means you are at higher risk. We should proactively manage this risk to reduce the likelihood of progression to glaucoma.
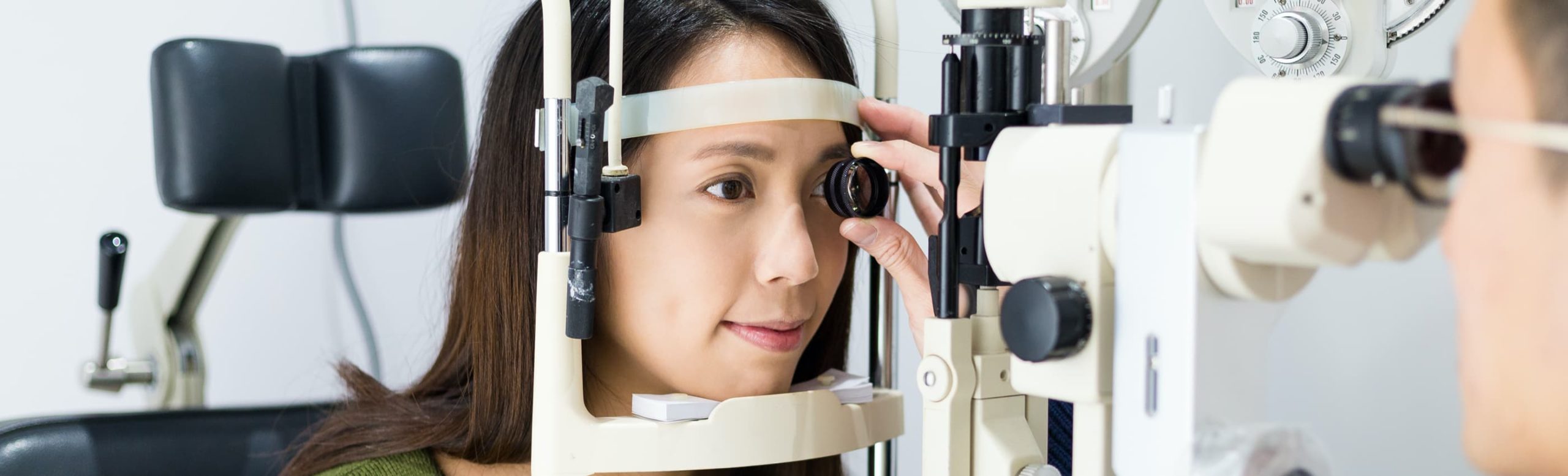
Symptoms of glaucoma
Symptoms depend on how advanced the glaucoma is and how high the eye pressure is.
Early glaucoma is asymptomatic. It is when you get to the advanced stage that you notice your peripheral vision has decreased. You may find yourself bumping into things, unable to see steps clearly, or having difficulty noticing incoming cars when you are crossing the road. By the time you reach this stage, your peripheral vision will almost certainly no longer be safe for driving.


Sometimes, acute glaucoma can occur when the eye pressure becomes very high (more than 40 mmHg). When this happens, your eye will become very red and painful. Your vision will be blurry and you will see haloes. You will most likely also experience a headache and nausea.
Types of glaucoma
There are quite a few types or classifications of glaucoma, but the underlying principle of optic nerve damage due to eye pressure remains the same, regardless of the type of glaucoma.
Open angle glaucoma refers to glaucoma that occurs with an open drainage angle, where there is no physical obstruction to aqueous draining out through the trabecular meshwork.
Angle closure glaucoma occurs when the iris obstructs the aqueous from draining out through the trabecular meshwork.
Normal tension glaucoma refers to glaucoma that occurs despite eye pressure being in the normal range (generally accepted as 8 to 21 mmHg).
Secondary glaucoma means that there is a known underlying cause for the high eye pressure. For example, you can get secondary glaucoma following trauma or prolonged use of steroid medication.
Pigmentary glaucoma is a type of secondary glaucoma where the eye pressure is high due to increased pigment in the eyeball. This increased pigment clogs up the trabecular meshwork and prevents aqueous from draining properly.
There are more types of glaucoma, but the most important thing to remember is that the main treatment goal is the same for all types of glaucoma – to reduce the eye pressure.
Yes, young people can get glaucoma, with the risk increasing with age. Approximately 1 in 10,000 babies develop glaucoma within 6 months of birth. At age 40, around 1 in 200 adults will develop glaucoma.
Glaucoma Melbourne
First-line treatment for glaucoma
The main goal of glaucoma treatment is to reduce the eye pressure.
The first-line treatment options for glaucoma are:
- Eye drops.
- Laser treatment (either selective laser trabeculoplasty or laser iridotomy).
Selective laser trabeculoplasty (SLT)
Selective laser trabeculoplasty (SLT) is performed to reduce eye pressure in open angle glaucoma. The laser stimulates cells in the trabecular meshwork to work harder to drain aqueous from the eyeball.
Most of the time, no eye drops are needed after SLT. However, if the SLT procedure incites more inflammation than usual, you will be given anti-inflammatory eye drops to use 3 times daily for 1 week.
Laser iridotomy
Laser iridotomy is performed to widen the drainage angle in angle closure glaucoma. The laser creates a hole in the iris, thus providing better access for aqueous to drain out via the trabecular meshwork.
After laser iridotomy, you will need to use anti-inflammatory eye drops 3 times daily for 1 week.
About laser treatment for glaucoma
Both SLT and laser iridotomy are performed in the rooms. The laser procedures take less than 5 minutes each to perform. Before laser treatment, eye drops are instilled to constrict your pupil. These drops can take up to 30 minutes to work and may blur your vision and cause a headache for a couple of hours.
Laser treatment is delivered through a special contact lens placed at the front of your eye. You will feel some discomfort during the procedure.
After laser treatment, you may have to wait 30 to 60 minutes to have your eye pressure rechecked before you go home.
After laser, you may experience some blurriness, irritation, and sensitivity to light. These symptoms will gradually improve over the next few days.
I generally perform the laser procedures one eye at a time, with laser to the second eye occurring a few weeks after the first. You will be reviewed 6 to 8 weeks after the laser.
Research :
Dr Brian Ang has published scientific papers on both selective laser trabeculoplasty and laser iridotomy.
Glaucoma surgery
Types of glaucoma surgery procedures
Most patients with glaucoma are treated with eye drops or laser, or a combination of both.
"In some patients however, these glaucoma treatments are not able to reduce the eye pressure enough. The pressure remains stubbornly high and the glaucoma continues to cause damage to the optic nerve. This is when glaucoma surgery becomes necessary."
Dr Brian Ang Glaucoma surgeon Melbourne
The 2 main reasons that I recommend surgery are:
- Uncontrolled eye pressure despite using maximum possible medical therapy and having undergone laser treatment
- Rapidly progressing glaucoma, where there is a significant risk of blindness if surgery is not performed
Trabeculectomy
Trabeculectomy is currently the gold standard surgery to reduce eye pressure. The surgery involves creating a drainage channel to allow aqueous to drain out from the eye into a ‘bleb’, which is a pocket of aqueous underneath the conjunctiva (skin of the eye).
The surgery is performed as a day case and will take 45 to 60 minutes to complete. Your postoperative reviews will be fairly regular in the first month. As the eye settles, additional procedures may be required, such as removal of sutures, laser to cut sutures, and injection of anti-scarring medication around the bleb. It can take a few months (and quite a bit of fluctuation in eye pressure) before the eye eventually settles.
Glaucoma damage is irreversible, so any vision loss from glaucoma cannot be recovered. The aim of surgery is to try to slow down glaucoma progression, and if possible, stop further damage from occurring altogether.
You will need to fast for at least 6 hours before surgery. If you are taking blood-thinning medications such as aspirin, clopidogrel or warfarin, please stop for 3 days prior to surgery, as long as you have received medical advice that it is safe to do so. This is to reduce the risk of uncontrolled bleeding during surgery.
No specific dietary changes are required beforehand. It is not strictly necessary to stop smoking, but stopping smoking may aid in the recovery process following surgery.
Glaucoma surgery is a day case procedure and is usually performed in day surgery under local anaesthesia. You will be awake during the surgery but you will be sleepy due to sedating medication that the anaesthetist gives you.
There will be a pad and shield placed over your eye, which can be removed the next day. When you remove the pad, your vision will be blurry, your eye will feel uncomfortable, and you may notice some double vision. This is a normal part of recovery. You will find that the vision will gradually improve over the next few weeks.
In general, there will be a first postoperative review the next day, and then weekly thereafter for 1 month.
You will have two different eye drops to use after surgery. The antibiotic is used 4 times daily, and can be stopped after 1 week. The steroid drop is used every 2 hours while awake, and will be gradually reduced over the next 3 to 4 months. You will no longer need to use your usual glaucoma medications in that eye.
Glaucoma surgery is not like cataract surgery. With glaucoma surgery, postoperative aftercare is also crucial to the success of the operation.
This is why additional procedures are often required to ‘adjust’ the postoperative recovery; these include:
- The removal of sutures
- Laser to cut sutures
- Injection of anti-scarring medication around the bleb
Also, please be prepared for fluctuations in eye pressure during the initial stages of recovery – sometimes the eye pressure can be too high or too low – this will eventually settle but can take a few months.
No. Glaucoma damage is irreversible, so any vision loss from glaucoma cannot be recovered. The aim of surgery is to try to slow down glaucoma progression, and if possible, stop further damage from occurring altogether.
Trabeculectomy has a success rate of around 70-80%. Most complications can be managed and do settle over time. Sight-threatening complications occur rarely (less than 1 in every 1000). These can sometimes occur even if the operation has been carried out perfectly. The main risks and complications of surgery include bleeding, infection, cataract, eyelid droop, eye pressure too low or too high, failure of surgery, the need to perform additional surgical procedures, and very rarely, blindness.
Glaucoma tube shunt implants
If trabeculectomy surgery has failed, glaucoma tube shunts are your next option. They are tubes that are implanted into the front part of the eye, through which aqueous drains out of the eye.

Glaucoma surgeon Melbourne
“In some cases, glaucoma tube shunts are implanted as first-line surgical treatment. For example, if you are at high risk of conjunctival scarring or if you are unable to undergo the intensive postoperative management that a trabeculectomy demands.”
In general, the recovery period after glaucoma tube shunt implantation is around 2 to 4 months.
The main benefit of the glaucoma tube shunt over trabeculectomy is that the postoperative management is not as intensive and is less susceptible to failure from scarring. This operation may therefore be suited to you if you live a long distance from care, or if you scar easily (meaning that trabeculectomy is very likely to fail if performed in your eye).
MIGS
In the last few years, a new class of treatment called minimally invasive glaucoma surgery (MIGS) is becoming increasingly popular.
MIGS can be performed as an independent procedure but is normally performed in conjunction with cataract surgery. It is ideal if you want to reduce the number of eye drops you use, or if you need your eye pressure reduced but are wary of the risks of traditional glaucoma filtering surgery.
The two commonest MIGS devices are the iStent and the Hydrus microstent. These tiny stents are implanted to help reduce eye pressure by assisting with aqueous drainage via the trabecular meshwork.
When combined with cataract surgery, there is no change to the way cataract surgery is performed. The stent is implanted after the artificial lens implant has been inserted. This adds an extra 5 to 10 minutes to the overall cataract surgery time without any significant added risk. These stents are MRI-safe.
Main advantages of MIGS compared to traditional glaucoma filtering surgery (trabeculectomy and glaucoma tube shunt):
- MIGS is less invasive
- MIGS is quicker to perform
- MIGS has a faster recovery period (of 4 to 6 weeks)
- MIGS has less risk of complications
Research : Dr Brian Ang has published scientific papers on trabeculectomy, glaucoma tube shunt surgery, and MIGS.
Glaucoma surgery costs
How much does glaucoma surgery cost?
The cost of glaucoma surgery depends on your health fund. There will be an out-of-pocket fee for the initial consultation, as well as for any other tests that may be required during the consultation (such as a visual field test and OCT scan).
In general, there will be a gap fee for the surgery and also for the anaesthetist. There may also be an initial excess fee charged by the health fund.
Please confirm with your health fund that you are covered for glaucoma surgery. The Medicare item numbers are 42746 (trabeculectomy), 42752 and 42662 (glaucoma tube shunt), 42504 (standalone MIGS stent implantation), and 42705 (MIGS stent implantation combined with cataract surgery).
The cost of glaucoma surgery for uninsured patients depends on a few things, including the choice of operating facility, the complexity of the surgery, and whether it is combined with another surgical procedure such as cataract surgery. The surgical bookings manager will be able to discuss costs in greater detail once you have had your comprehensive eye examination.
Benefits of private glaucoma surgery
The main benefit of doing your glaucoma surgery privately is that you know who will be performing your surgery and managing your postoperative visits. Vice versa, the glaucoma specialist knows you and your individual case.
With public hospitals, surgery is free but you cannot choose your surgeon or the doctors you see during your follow-up visits. Furthermore, not all public hospitals offer glaucoma surgery and those that do often have a long waiting list.
Private glaucoma surgery can usually be scheduled within 3 to 4 weeks, or even on the same day, if urgent.